COCONUT AND ITS ANTI-BACTERIAL FUNCTIONS
Lauric acid, the major fatty acid from the fat of the coconut, has been recognized for its unique properties in food use, which are related to its antiviral, antibacterial, and antiprotozoal functions. Desiccated coconut is about 69% coconut fat, as is creamed coconut. Approximately 50% of the fatty acids in coconut fat are lauric acid. Lauric acid is a medium chain fatty acid, which has the additional beneficial function of being formed into monolaurin in the human or animal body. Monolaurin is the antiviral, antibacterial, and antiprotozoal monoglyceride used by the human or animal to destroy lipid-coated viruses such as HIV, herpes, cytomegalovirus, influenza, various pathogenic bacteria, including listeria monocytogenes and helicobacter pylori, and protozoa such as giardia lamblia. Some studies have also shown some antimicrobial effects of the free lauric acid.
Also, approximately 6-7% of the fatty acids in coconut fat are capric acid. Capric acid is another medium chain fatty acid, which has a similar beneficial function when it is formed into monocaprin in the human or animal body. Monocaprin has also been shown to have antiviral effects against HIV and is being tested for antiviral effects against herpes simplex and antibacterial effects against chlamydia and other sexually transmitted bacteria.
Adapted from: Coconut: In Support of Good Health in the 21st Century by Mary G. Enig, Ph.D., F.A.C.N.
Full story: http://coconutoil.com/coconut_oil_21st_century
MONOLAURIN AND AIDS
Monolaurin is an antiviral, antibacterial, and antiprotozoal monoglyceride that your body makes from the lauric acid in the fat in motherís milk, in cowís milk, and lauric fats such as coconut oil and palm kernel oil. The largest and easiest source of lauric acid is coconut oil (and or course whole coconut products). There is extensive scientific literature on its efficacy. Lauric acid is turned into monolaurin in the gut and this is what keeps infants fed human milk from getting sick even when they exposed to lipid coated viruses and various pathogenic organisms.
The AIDS virus is killed by monolaurin. Why it is not more extensively used is probably related to the fact that most people donít understand what it does and why it does it, even when you explain the effects. There have been some reported benefits for several years from both monolaurin capsules and coconut; however, this has all been anecdotal reporting and there have not been any properly conducted clinical trial.
Source: Know Your Fats. The Complete Primer for Understanding the Nutrition of Fats, Oils and Cholesterol. Enig, Mary, G. Ph.D. 2000.
COCONUT AS THE NATURAL SOURCE OF LAURIC ACID
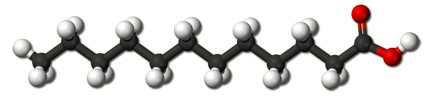
Lauric acid or dodecanoic acid, its chemical name, is the most potent fatty acid there is. Most of it is naturally found in coconut oil. More than half of the fatty acids found in coconut oil is lauric (C12). Together with caprylic acid (C8) and capric acid (C10), these three make up the medium chain fatty acid (MCFA) content of coconut oil.
MCFAs are the “antimicrobial powerhouse” behind coconut oil’s ability to cure and prevent a growing list of disease and illness. Lauric, capric and caprylic acids and their respective monoglycerides, monolaurin, monocaprin and monocaprylin, all exhibit antimicrobial activity that boosts your immune system. Of all the MCFAs, lauric (C12) acid appears to have the greatest overall effect.
Below are just some of the microorganisms destroyed by this mighty MCFA.
- AIDS virus (HIV)
- Chlamydia pneumoniae
- Herpes simplex virus II
- Gram-positive organisms
- Hepatitis C virus
- Group A, B, F, and G streptococci
- Helicobacter pylor
- Measles virusi
- Listeria monocytogenes
- Leukemia virus
- Streptococcus agalactiae
- Influenza virus
- Staphylococcus aureus
- Epstein-Barr virus
- Hemophilus influenzae
- Sarcoma virus
- Escherichia coli (E. coli)
Lauric acid is not just about killing bacteria, viruses, fungi and other harmful organisms. This magnificent MCFA tends to improve cholesterol ratio by increasing HDL (good) cholesterol. It also enhances the ability of your pancreas to secrete insulin.

COCONUT OIL HAS LOWER FAT CALORIES THAN OTHER OILS AND FATS
Coconut oil is the world’s only, low calorie fat. Coconut oil has at least 2.56% fewer calories per gram of fat than other fats and oils. The coconut oil contains only 6.8 calories per gram versus 9 calories per gram for other oils. It is unique among oils in that it promotes weight loss.
Coconut oil is thermogenic. The special fats in coconut oil called medium chain fatty acids (MCFAs) are not stored in your body as fat. It raises the bodyís metabolism, and even prevents the accumulation of fat by burning calories and converting fat into energy. Coconut oil is natural fat burner and bodyís energy booster since its digestion is different from that of carbohydrates and bodyís energy booster since its digestion is different from that of carbohydrates and protein. It is ideal for weight loss.
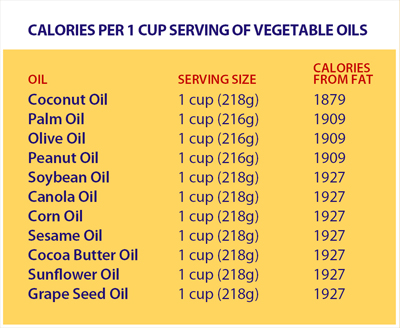
Source: COCONUT: PHILIPPINES. Villafuerte-Abonal, Lalaine. 2007.
HEALTH FACTS ABOUT COCONUTS
- Coconut oil has lower calories than any other fats.
- MCFAs in coconut oil promote thermogenesis which increases the bodyís metabolism.
- MCFA in coconut oil is faster to digest and has better solubility in biological fluids.
- Coconut oil is used to facilitate absorption of calcium and magnesium, both of which are essential for bone development.
- MCFA in coconut oil can destroy illness-causing viruses, fungi and bacteria easily on contact similar to the colostrums of motherís milk.
- Lauric acid in coconut oil is good for geriatic patients as it contributes to faster surgical recovery.
- MCFAs in coconut oil can kill gram-positive cocci.
- Capric and lauric acid in coconut oil can kill Candida albicans, a common yeast infection found in those who have used antibiotic excessively.
COCONUT CONTAINS ZERO TRANS FATS
What is trans-fat?
Trans-fat, also called Trans fatty acids (TFA), is formed when hydrogen is added to a vegetable oil to make a more solid fat like shortening or margarine. This process is called hydrogenation, and it is used to increase the shelf life and maintain the flavor and texture of foods.
Trans-fats behave like saturated fats by raising the ìbadî cholesterol, low-density lipoprotein (LDL), which may increase risk of coronary heart disease (CHD), a leading cause of death in the United States.
Source: Trans Fat Fact Sheet. USDA. http://www.fns.usda.go
Full story: http://www.fns.usda.gov

COCONUT IS GOOD FOR DIABETICS
Blood sugar is an important issue for anyone who is concerned about heart disease, overweight, hypoglycaemia, and especially diabetes because it affects all of these conditions.
Carbohydrates in our foods are broken down in the digestive tract and converted into glucose (blood sugar). Meals that contain a high concentration of carbohydrates, particularly simple carbohydrates such as sugar and refined flours, cause a rapid rise in blood sugar. Since elevated blood sugar can lead to a coma and death, insulin is frantically pumped into the blood stream to avoid this. If insulin is produced in adequate amounts blood sugar is soon brought back down to normal. This is what happens in most individuals. However, if insulin is not produced quickly enough or if the cells become desensitized to the action of insulin, blood glucose can remain elevated for extended periods of time. This is what happens in diabetes.
Dietary fiber helps moderate swings in blood sugar by slowing down the absorption of sugar into the blood stream. This helps keep blood sugar and insulin levels under control. Coconut fiber has been shown to be very effective in moderating blood sugar and insulin levels. For this reason, coconut is good for diabetics.
Diabetics are encouraged to eat foods that have a relatively low glycemic index. The glycemic index is a measure of how foods affect blood sugar levels. The higher the glycemic index, the greater an effect a particular food has on raising blood sugar. So diabetics need to eat foods with a low glycemic index. When coconut is added to foods, including those high in starch and sugar, it lowers the glycemic index of these foods. This was clearly demonstrated by T. P. Trinidad and colleagues in a study published in the British Journal of Nutrition in 2003. In their study, both normal and diabetic subjects were given a variety of foods to eat. Some of the types of food included cinnamon bread, granola bars, carrot cake, and brownies, all foods that a diabetic must ordinarily limit because of their high sugar and starch content. It was found that as the coconut content of the foods increased, the blood sugar response between the diabetic and non-diabetic subjects became nearly identical. In other words, coconut moderated the release of sugar into the bloodstream so that there was no spike in blood glucose levels. As the coconut content in the foods decreased, the diabetic subjectsí blood sugar levels became elevated, as would normally be expected from eating foods high in sugar and white flour. This study showed that adding coconut to foods lowers the glycemic index of the foods and keeps blood sugar levels under control. Sweet foods such as cookies and cakes made using coconut flour do not affect blood sugar levels like those made with wheat flour. This is good news for diabetics who want a treat now and then without adversely affecting their blood sugar.
Source: Coconut Flour: A Low Carb, Gluten-Free, Alternative to Wheat by Bruce Fife, ND.
Full story: http://www.coconutresearchcenter.org/newsletter-sample.htm
CAN COCONUT OIL BE ATHEROGENIC?
According to the universally accepted Lipid-Heart Theory, high saturated fats cause hypercholesterolemia and coronary heart disease. Coronary morbidity and mortality are said to be highest in the countries and peoples consuming the highest amounts of saturated fats. Coconut oil, with its saturated medium chain fats, has been especially condemned for this reason. The true facts are just the opposite. The countries consuming the highest amounts of coconut oil ñ the Polynesians, Indonesians, Sri Lankans, Indians, Filipinos ñ have not only low serum cholesterol but also low coronary heart disease rates – morbidity and mortality.
The reason why coconut oil cannot be atherogenic is basic. Coco oil consists predominantly of 65% medium chain fatty acids (MCFA) and MCFAs are metabolized rapidly in the liver to energy and do not participate in the biosynthesis and transport of cholesterol. Coconut oil, in fact, tends to raise the HDL and lower the LDL:HDL ratio. Coco oil is not deposited in adipose tissues and therefore does not lead to obesity. It is primarily an energy supplier and as fast a supplier of energy as sugar.
MCFAs therefore differ in their metabolism from all the long chain fatty acids, whether saturated or unsaturated.
The pathogenesis of atherosclerosis has recently taken a complete paradigm shift – from a simple deposition of cholesterol and cholesterol esters to an inflammatory condition where numerous genetically dependent factors – dyslipoproteinemias, dysfunctions of endothelial and other cells leading to invasions of the subendothelial region by macrophages, smooth muscle cells, leukocytes and T cells ñ all interplay in a scenario still not fully understood. This will be discussed at length and whatever role fat deposition plays appears late in atherogenesis and secondary to oxidation process and the overriding role of the dysfunctional endothelium. Coconut oil has no role at all to play in this highly complex and still ill understood process.
Adapted from: COCONUT OIL: Atherogenic or Not? By Conrado S. Dayrit, MD, FPCC, FPCP, FACC. Philippine Journal Of Cardiology. July-September 2003, Volume 31 Number 3:97-104.
Full story PDF: http://www.coconutoil.com/DayritCardiology.pdf

COCONUT CONTAINS HIGH AMOUNT OF DIETARY FIBER
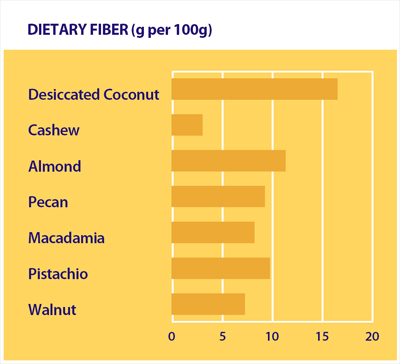
HEALTH BENFITS OF DIETARY FIBER
- Aids weight control and reduces risk of developing obesity.
- Forms a vital part of the diet by adding mass to the stool which eases elimination.
- Soluble dietary fibers can be useful for controlling blood glucose in patients with diabetes.
- Soluble dietary fiber also inhibits cholesterol absorption from small intestines thereby reducing serum cholesterol.
- Plays a key role in preventing cancer of the large intestines commonly called colon cancer.
Sources: USDA National Nutrient Database for Standard Reference Release
COCONUT FOR WEIGHT MANAGEMENT
Effects of dietary coconut oil on the biochemical and anthropometric profiles of women presenting abdominal obesity.
Assunão ML, Ferreira HS, dos Santos AF, Cabral CR Jr, Florêncio TM.
Faculdade de Nutricão, Universidade Federal de Alagoas, Maceió, AL 57072-970, Brazil.
Abstract
The effects of dietary supplementation with coconut oil on the biochemical and anthropometric profiles of women presenting waist circumferences (WC) >88 cm (abdominal obesity) were investigated. The randomised, double-blind, clinical trial involved 40 women aged 20-40 years. Groups received daily dietary supplements comprising 30 mL of either soy bean oil (group S; n = 20) or coconut oil (group C; n = 20) over a 12-week period, during which all subjects were instructed to follow a balanced hypocaloric diet and to walk for 50 min per day. Data were collected 1 week before (T1) and 1 week after (T2) dietary intervention. Energy intake and amount of carbohydrate ingested by both groups diminished over the trial, whereas the consumption of protein and fiber increased and lipid ingestion remained unchanged. At T1 there were no differences in biochemical or anthropometric characteristics between the groups, whereas at T2 group C presented a higher level of HDL (48.7 +/- 2.4 vs. 45.00 +/- 5.6; P = 0.01) and a lower LDL:HDL ratio (2.41 +/- 0.8 vs. 3.1 +/- 0.8; P = 0.04). Reductions in BMI were observed in both groups at T2 (P < 0.05), but only group C exhibited a reduction in WC (P = 0.005). Group S presented an increase (P < 0.05) in total cholesterol, LDL and LDL:HDL ratio, whilst HDL diminished (P = 0.03). Such alterations were not observed in group C. It appears that dietetic supplementation with coconut oil does not cause dyslipidemia and seems to promote a reduction in abdominal obesity.
Source: Pubmed. US National Library of Medicince. http://www.ncbi.nlm.nih.gov/pubmed/19437058
Full story: http://www.ncbi.nlm.nih.gov/pubmed/19437058

Coconut Products and Their Uses
Each component of the coconut, from husk and fiber to the natural extracts has an extremely valuable route to market, which contributes to increasing the value of the crop. Able to outlive any man who plants it, the coconut tree’s ability to supply an abundance of essential nutrients has earned it the titles of 'Jewel of the Tropics', 'King of Trees' and 'The Tree of Life'. Some of the most valuable products are gathered below, but the list is by no means comprehensive.
Activated Carbon Filtration
Extensive research in this field is producing multiple industry applications for activated carbon produced from coconut husks and shells. Traditional uses in water purification for both groundwater and drinking water filtration are being joined by applications in nuclear plants, solvent recovery and utilization in catalytic converters.
- A high carbon content makes coconut shells a perfect source to produce activated carbon
- Coconut based activated carbon has the most microporous pore structure, and has the highest hardness compared to other types of activated carbon. This makes it the best carbon for water filtration
- It generates the least ash during production
- The carbon can be reactivated
Lauric Acid
Coconut Oil contains 50% lauric acid, most commonly used in soap production and manufacturing cosmetics. In humans, lauric acid is converted into monolaurin, a compound which has antiviral, antimicrobial and antifungal properties.
Biodiesel
Coco-Biodiesel is created by processing pure coconut oil and converting it to a diesel-like product. It is set to become a more prominent part of the worldwide biofuel blend as pressure mounts on international governments to employ cleaner burning and non-toxic alternative fuels from renewable sources. Biodiesels will reduce greenhouse gas emissions, and can be used in diesel engines without modifications.
- Brazil is one of the world’s largest biofuel consumers and has 10 million flex-fuel cars on its roads
- The global consumption of ethanol and biodiesel is projected to reach 135 billion gallons by the year 2018
- Coconut oil burns more slowly than diesel engines, reducing engine wear and lubricating the engine more efficiently
Fibers
Coconut husk fibers, also known as coir, come from the large outer casing that surrounds the hard brown nut. These tough fibers are used to make mats, packaging, mattresses and brushes. It can even be rubberized and used as an eco-friendly alternative to plastics, an application car manufacturer Ford is currently researching.
Husks and Shells
The husks and shells have historically been used as charcoal and as a potting medium for growing saplings. However, the most recent demand, and one that looks set to grow, is the use of the husks and shell as biomass fuel.
- Biomass energy is responsible for over 75 per cent of the world’s renewable energy, and demand for woody biomass is increasing rapidly
- Global demand for biomass products is estimated to increase by 600 per cent over the next 20 years, according to the International Institute for Environment and Development
Milk
Coconut milk is made by pressing the flesh of the coconut or by passing hot water or milk through grated coconut.
There is a high demand for this product within the food industry, particularly in the Asian market where it features in many traditional dishes.
The milk is a premium cooking product in Western markets and is being added to shopping baskets more readily as consumers develop a taste for Eastern flavors.
Water
The sweet water from young coconuts is a refreshing, nutrient-packed liquid ubiquitous in tropical countries like Brazil, Indonesia and India where coconut trees are indigenous.
Coconut water is expanding beyond its traditional markets. Beverage giants PepsiCo and Coca-Cola, and a host of smaller niche suppliers, are promoting the product to a wider global market.
- The latest available data shows that the market for coconut water in key demographics grew by 26% annually between 2007-11
- Although still in its infancy, the coconut water market in the United States was valued at $350m in 2012 and continues to experience super-normal growth
- Brazil, with the world’s fifth biggest population (196m people), is the largest market for packaged coconut water, where it accounts for 70% of total beverage volume sales
- More than 200 brands are now in the global marketplace, including major players Vita Coco, Zico (Coca-Cola has a stake in the company) and O.N.E. (PepsiCo's investment). PepsiCo also owns Amacoco, Brazil's largest coconut water producer
- Celebrities have played a major role in boosting the commercial profile of coconut water brands; Vita Coco has chosen Rihanna to front its international marketing and Madonna has invested directly in the company.
Oil
Coconut oil is a stable and well-established commodity that has been traded globally for more than fifty years.
Extracted from the dried white flesh of the coconut, coconut oil is a multi-purpose liquid that can be used as a cholesterol cutting cooking oil, healthcare product and biofuel feedstock.
- The oil is anti-viral, anti-bacterial, anti-fungal and anti-microbial
- Coconut oil products have been shown to tackle Alzheimer’s, tooth decay and all manner of medical conditions
- It is increasingly popular in the pharmaceutical industry which is ploughing millions of dollars into further research of its medicinal properties
- The price of coconut oil has more than doubled over the last decade and exports of virgin coconut oil to major Western markets have doubled in the last year

Coconut Oils
Refined Coconut Oil vs. Virgin Coconut Oil
There are two broad categories of coconut oils: those that are mass produced at an industrial level and need to be refined, and those that start with fresh coconut and have much less refining. Yes, you read that correctly, less refining.
Coconut oil by nature is a refined product, because oil does not grow on a tree. Coconuts do. All coconut oils have to be extracted from the whole coconut, therefore technically speaking, the only truly “unrefined” coconut oil you can consume is the oil still inside the coconut meat from a fresh coconut just picked off the tree.
The term that is used for the least refined coconut oils is “virgin coconut oil.” Using similar terminology as is used with other edible oils, the term “virgin” was used with coconut oil back in the early 2000s to designate the least refined coconut oils in the market.
The definition for “virgin” coconut oil was originally developed in an Internet discussion group we hosted, and various people had input into the definition, including industry insiders, academic leaders, and others. The definition we all agreed upon at that time, was that “virgin” coconut oils would be coconut oils produced without dried “copra” as its starting point.
“Copra” is an industry-defined term used in the Philippines to refer to dried coconut that has been removed from the coconut shell, but which by itself is inedible and needs to be further refined to produce coconut oil. Copra can be produced in several ways, including smoke drying, sun drying, or kiln drying, or derivatives or a combination of any of these methods. The one thing they have in common, is that the product at that point is not suitable for consumption and must be further refined. It’s smokey, it’s dirty – it’s certainly nothing that resembles a food when it is in the form of copra. Copra is a kind of commodity, with its own market price, separate from coconuts, or coconut oil (the finished product). There are traders and dealers of copra in coconut producing countries, and they sell their copra to coconut oil manufacturing plants. Copra is even exported to countries like the U.S., where it is further refined for industrial uses.
Refined Coconut Oils
In the coconut producing countries, these copra-based refined coconut oils are usually referred to as “RBD coconut oils.” RBD stands for: refined, bleached, deodorized. The “bleaching” is generally not a chemical process, but rather a filter process to remove impurities. A “bleaching clay” is used for this filtering. Steam is used to deodorize the oil, since the starting point was copra. So the resulting product has a very bland taste, with little or no odor.
One of the misconceptions propagated on the Internet is that only virgin coconut oils are healthy, while refined coconut oils are not, and that they actually might be harmful. This is generally untrue, with a couple of exceptions that I will explain below. These RBD coconut oils have been in the market for many years now, and are the primary dietary oils consumed by billions of people in tropical climates around the world. The RBD refining process does nothing to alter the fatty acid profile of coconut oil, so all the medium chain fatty acids are kept intact.
What the refining process does do, however, is strip away some of the nutrients. Virgin coconut oils are tested higher in antioxidants, for example. But this fact does not make RBD refined coconut oils “unhealthy”.
The types of refined coconut oils one currently finds on the market include:
Expeller-pressed Coconut Oils: These are typically RBD coconut oils produced in tropical countries through mechanical “physical refining” from copra. Physical refining is considered “cleaner” than chemical refining that uses solvent extracts like “hexane”.
Coconut Oil: If no description is given and just the plain term “coconut oil” is used, it is probably an RBD coconut oil. It should be noted that copra is a product that is exported to the United States, where companies refine it into non-edible uses. Cleaning products and detergents are a common use, for example. Now, with the rise of popularity of coconut oil as an edible oil again, some of these large U.S. manufacturing companies are beginning to package coconut oil as an edible oil. These cheaper oils are more than likely mass produced with solvent extracts. We are not aware if any of these solvents remain in the finished product, but if you want to be sure, try to purchase a refined coconut oil that has been refined without them.
Hydrogenated Coconut Oil: This is the one refined coconut oil you want to stay away from as an edible oil. The small portion of unsaturated fatty acids are hydrogenated, creating some trans fats. It also keeps coconut oil solid at higher temperatures. We are not aware of such a product in the U.S. edible oil market at this time. If it exists as a product, it is probably going to be as an ingredient in the confection industry in tropical climates. Standard RBD coconut oil remains solid up to 76 degrees F., and the ambient air temperature is higher than that in the tropics most of the time. So to keep coconut oil solid at higher temperatures, they hydrogenate it before putting it into candies or baked goods, or making into margarines.
Liquid Coconut Oil: A new product that appeared in stores as an edible oil in 2013 was “liquid coconut oil” that is promoted as “coconut oil that stays liquid even in your refrigerator”. It may be a new label and a new item in the edible oil section, but the product is not new at all. It is “fractionated coconut oil” that has had lauric acid removed. It is also referred to as “MCT oil“. It has typically been used in the past in skin care products, and more recently as a dietary supplement. It is a refined product that is now marketed as an edible oil. It is actually a by-product from the lauric acid industry. Lauric acid from coconut oil is known as a strong antimicrobial component, and therefore used as a preservative in many commercial applications. Being a saturated fatty acid, and comprising about 50% of coconut oil, once it is removed you are left with a liquid oil with a much lower melting point. So if you see this product online or in a store, just be aware that it is a highly refined product, and that it is missing coconut oil’s star component: lauric acid.
Virgin Coconut Oils
Let’s now turn to “virgin coconut oils”. As I mentioned above, the common denominator that should exist in all virgin coconut oils is that they start with fresh coconut and not copra. However, there is no worldwide certification body that determines or certifies coconut oils as “virgin”, so anybody can use the term and put it on a label if they so choose. The first thing to investigate when choosing a virgin coconut oil, is whether or not it is actually a copra-based coconut oil or not. If it does use copra as its starting point, it really is not a true virgin coconut oil, but an industry standard RBD refined coconut oil with a clever label.
Extra Virgin Coconut Oil
A common title or term used is “extra virgin coconut oil”. So what is the difference between “virgin” and “extra-virgin” coconut oil?
Nothing. There are no commonly understood or accepted definitions for “extra” virgin coconut oil, as there are in the olive oil industry. It is simply a marketing term and nothing else.
So in analyzing the virgin coconut oils that are currently in the market, which would also include those coconut oils labeled as “extra virgin”, we see that all virgin coconut oils fall into two broad methods of production:
1. Virgin coconut oil derived from pressing the oil out of dried coconut. In this method, the fresh coconut meat is dried first, and then later the oil is pressed out of the coconut. This method allows for easier mass production of virgin coconut oil. Since the dried coconut (desiccated coconut) industry is well established in coconut producing countries, many of these industries have added virgin coconut oil to their product line.
This is the most common type of “virgin” or “extra virgin” coconut oil that you will find online and in stores today. It is mass-produced, but it is a higher quality oil than RBD coconut oil, as it starts with fresh coconut and not copra.
2. Virgin coconut oil derived through a “wet-milling” process. With this method, the oil is extracted from fresh coconut meat without drying the coconut meat first. “Coconut milk” is expressed first by pressing it out of the wet coconut meat. The oil is then further separated from the water. Methods which can be used to separate the oil from the water include boiling, fermentation, refrigeration, enzymes, and mechanical centrifuge.
We are very fortunate today that the coconut oil producing countries have done quite a bit of research on virgin coconut oils over the past several years. They have begun to wake up to the fact that Western advice on dietary oils, which has led to the demonization of their traditional fats and oils like coconut oil, has been primarily political in nature, rather than scientific.
Much of their research in recent years has been in the area of cholesterol and heart disease, since this is the main point of attack from Western countries. They have learned that their traditional fats and oils are actually healthier than the newer expeller-pressed seed oils from soy and corn, two crops heavily subsidized by the U.S. government which keeps prices artificially low. We feature much of this research on our peer-reviewed research page at CoconutOil.com. This research has confirmed that not only does virgin coconut oil NOT affect cholesterol levels negatively, but that it affects them positively. For more on this topic, see: Coconut Oil is Beneficial for Your Heart: Shining the Truth on Mainstream Media’s Negative Attacks Against Coconut Oil.
Researchers from universities in the Philippines, Malaysia, Sir Lanka, and India have looked at various methods of producing coconut oil. In the beginning, it was difficult to determine what could be measured in a laboratory to determine if virgin coconut oil was indeed superior to regular RBD refined coconut oils. They soon discovered that the one characteristic that could be measured, and that was significantly higher in virgin coconut oils than RBD refined coconut oils, was the level of antioxidants. Antioxidants were found to be much higher in the virgin coconut oils, especially those produced by the wet-milling method, as described above.
The Research on Wet-Milling Virgin Coconut Oil
The “wet-milling” process of producing virgin coconut oil, as explained above, extracts the coconut oil from a wet emulsion, or “coconut milk”. It does not press the oil out of dried coconut.
So which wet-milling process produces the highest quality virgin coconut oil? According to several studies, the fermentation wet-milling process, which uses heat, produces the highest levels of antioxidants in virgin coconut oil. The fermentation process is a simple technique of extracting coconut oil, much as has been done in people’s kitchens in tropical climates for hundreds of years.
During the fermentation process, a coconut milk emulsion is made from freshly grated coconut. Then the coconut milk is allowed to sit and ferment for a period of time, usually overnight. The heavier water sinks to the bottom of the container, leaving a crystal clear layer of oil on top, along with some coconut solids. This oil is then scooped out and put into a pan, like a large wok, and heated for a period of time until the coconut solids fall to the bottom of the pan. It is then filtered.
The first study examining virgin coconut oil production methods was published in 2008. This study was conducted in Malaysia and published in the International Journal of Food Science Nutrition. It was the first study reporting that the wet-milling fermentation method produced the highest amounts of antioxidants.
In 2011, studies conducted in Sri Lanka by Professor Kapila Seneviratne of the University of Kelaniya also showed that traditionally made wet-milling virgin coconut oils have the highest levels of antioxidants.
What was surprising about Seneviratne’s studies was the discovery that high levels of heat actually increased the amount of antioxidants in the coconut oils. This was surprising because there was a misunderstanding that heat supposedly was detrimental to coconut oil processing, as many virgin coconut oils in the market were claiming they were “raw” or “cold pressed” and did not use any heat. Here is what they wrote in The Sunday Times of Sri Lanka:
More surprises awaited the research team. The general impression is that cooking at high temperatures would degrade the quality of the oil. However, it is not applicable since coconut oil is thermally stable, it is learnt. “Fortunately, most of the phenolic anti-oxidants present in coconut oil are also thermally highly stable,” he pointed out, explaining that the reason for a greater composition of anti-oxidants is that simmering for a long time at a high temperature dissolved more anti-oxidants into the oil. (Published in The Sunday Times of Sri Lanka, October 16, 2011 – “Coconut Oil: It’s good for your after all,” by Kumudini Hettiarachchi and Shaveen Jeewandara)
In 2013, another study conducted in India also showed that virgin coconut oils produced by wet-milling and using heat produce higher levels of antioxidants. The study compared “cold extracted virgin coconut oil” (CEVCO) with “hot extracted virgin coconut oil” (HEVCO) and standard refined coconut oil (CCO) and was published in the journal Food Science and Biotechnology. Their testing showed that the “antioxidant activity in the HEVCO group was 80-87%, 65-70% in CEVCO, and 35-45% in CCO.” The researchers went on to comment why heat is necessary to produce the highest amounts of antioxidants in virgin coconut oil:
The increased polyphenol level in the HEVCO group may be due to increased release of bound polyphenols by heating. Coconut milk is an emulsion of oil and water that is stabilized by protein. To recover the oil from coconut milk, the protein bond has to be broken by heat in a double walled boiler known as a VCO cooker (steam jacket vessel developed by Central Plantation Crops Research Institute) under slow heating to allow the protein to coagulate and release the oil.”
So virgin coconut oils produced by wet-milling and being marketed as “no heat” or “raw” or “cold-pressed” are actually virgin coconut oils with lower levels of antioxidants, according to this body of research.
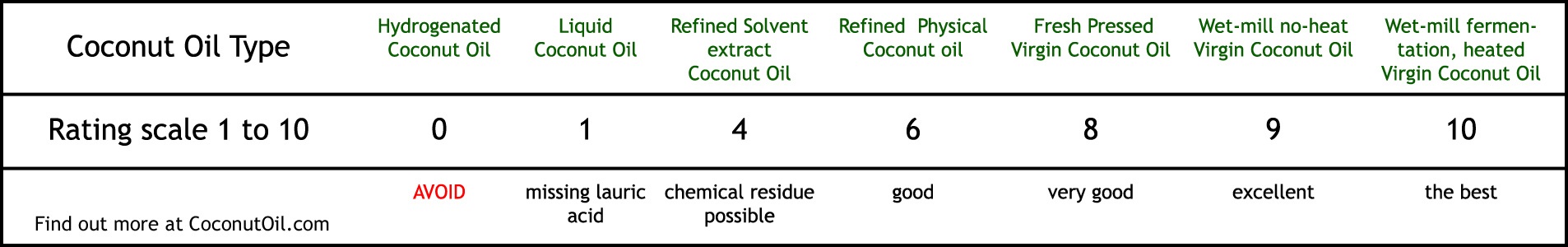
Source: by Brian Shilhavy
Full story: http://healthimpactnews.com/2014/what-type-of-coconut-oil-is-best-how-to-choose-a-coconut-oil/
Coconut Oil Vs
Coconut Oil Vs. Coconut Milk
Coconut oil and coconut milk both come from the meat of the coconut; however, coconut oil is extracted from the coconut meat, while coconut milk is made from the liquid that comes from grated coconut meat and is mixed with water. Both coconut oil and coconut milk contain healthy short and medium chain fatty acids like Lauric acid. Both contain vitamin E and K, and iron. It is recommended that adults have about 24 grams of Lauric acid daily; this equates to 3.5 tablespoons of an unrefined coconut oil or about 10 ounces of a good quality coconut milk. Coconut milk contains fewer calories than coconut oil does; a tablespoon of coconut milk contains around 30 calories, while a tablespoon of coconut oil contains around 115 calories.
Both coconut oil and coconut milk can easily be added into a daily diet; however, coconut oil is far more versatile than coconut milk is. Coconut oil can be used as cooking oil, in baking and can be taken straight as a daily health supplement. Coconut milk can be drank straight, added to sauces and stews, or added to milkshakes and smoothies. Coconut oil is used topically as a skin and hair care products, while coconut milk generally is not.
Coconut Oil Vs. Coconut Water
Coconut oil and coconut water both come from coconuts. However, coconut oil is made from mature coconuts, while coconut water is obtained from immature green coconuts. Coconut water does not contain all the medium chain healthy fatty acids that coconut oil contains; however, it contains health benefits that coconut oil does not contain. Coconut water is much like a sports energy drink, but it’s all natural. Coconut water contains electrolytes, water and carbohydrates, and helps to restore and rehydrate the body’s balance after exercise. Coconut water is also used as a fasting cleanser, and helps to keep the bowels clean and functioning properly. Coconut oil contains healthy medium chain fatty acids, vitamin K and E, and iron; it is used as a daily health supplement, as cooking oil and a baking substitute, and as a skin and hair care product. Both coconut oil and coconut water contain many health benefits; they are both excellent in their own way.
Coconut Butter Vs. Coconut Oil
Both coconut butter and coconut oil are made from the meat of mature coconuts. However, coconut oil is made by extracting it from the coconut meat, while coconut butter is made from the coconut meat being dried and then ground up. Both coconut oil and coconut butter should contain no other ingredients, but coconut; they should not even have water added. Coconut butter is about 70% coconut oil. When compared nutritionally, they are both excellent; they both contain healthy medium chain fatty acids, vitamin E and K, and iron. One tablespoon of coconut oil contains around 120 calories, while one tablespoon of coconut butter contains about 95 calories. Coconut oil contains no fiber, protein or carbohydrates, while one tablespoon of coconut butter contains 1.3 grams of fiber, 3.3 grams of carbohydrates and 0.9 grams of protein.
Coconut oil can be used as cooking oil for stir-fries and sauteing, a substitute for lard, butter, margarine or shortening in baking, as a daily health supplement and as a skin and hair care product. Coconut butter does not make a good cooking oil as it burns too easily, but makes an excellent skin and hair care product, can be used as a daily health supplement, and is excellent in drinks. Coconut butter can be easily transformed in to coconut milk by adding water.
Coconut Manna Vs. Coconut Oil
Coconut manna is basically coconut cream or coconut butter that the Nutiva company decided to give a different name to. Coconut manna is made from the meat of the coconut and contains no other ingredients, but coconut. Unlike coconut oil that makes an excellent cooking oil, coconut manna is not suitable for frying and sauteing as it burns too easily. Like coconut oil, coconut manna is packed full of healthy medium chain fatty acids, and makes an excellent daily health supplement. Both coconut oil and coconut manna are excellent skin moisturizers and help to reduce the look of wrinkles, stretch marks and scars.
Coconut Oil Vs. Coconut Cream
Coconut cream is the same as coconut butter. Both coconut oil and coconut cream are made from the meat of the coconut; however, coconut cream is made from the coconut meat being dried and ground up, while coconut oil is made by extracting it from the coconut meat. Both coconut cream and coconut oil have healthy medium chain fatty acids like Lauric acid, Capric acid and Caprylic acid. Both have antibacterial, antifungal, antioxidant and antimicrobial properties. Both coconut oil and coconut cream can be taken as a daily health supplement and can be used as a skin and hair care product. However, coconut cream cannot be used as cooking oil the way coconut oil can. Coconut cream can be used to make ice cream, pudding and is delicious on top of berries and other fruits.
Coconut Oil Vs. Canola Oil
Both coconut oil and canola oil comes from plants; coconut oil comes from coconuts and canola oil comes from the canola plant. The canola plant is a GMO plant that is derived from the rapeseed plant that is commonly used as a pesticide. Both coconut oil and canola oil contain vitamin K and E; however, canola oil contains significantly more. Canola oil contains healthy omega -3, but also contains a large amount of unhealthy omega-6. Coconut oil does not contain omega-3, but it contains medium chain fatty acids like Lauric acid, Capric acid and Caprylic acid. One cup of canola oil contains 1927 calories, while one cup of coconut oil contains 1879 calories. Between the two, coconut oil has more health benefits than canola oil has, and is a healthier cooking oil. Coconut oil is also far more versatile than canola oil is, as it can be used as a cooking oil, in baking, as a skin and hair care product and as a daily health supplement; canola oil is only used as a cooking oil.
Coconut Oil Vs. Olive Oil
Coconut oil is made from the meat of fresh coconuts, while olive oil is made from olives. There are many different grades of both olive oil and coconut oil; both types come in virgin, extra virgin, refined, unrefined, organic and non-organic. Both coconut oil and olive oil have numerous health benefits and are considered healthy cooking oils. Both olive oil and coconut oil contain healthy fats and both have excellent anti-oxidant properties, especially when they are in their pure natural forms. When compared on health benefits alone, coconut oil is slightly better than olive oil; however, olive oil is the far more popular cooking oil of the two. Both coconut oil and olive oil can be used as a cooking oil for stir-fries and sautéing. Both can also be used as a deep conditioner for hair. Coconut oil is a more versatile oil than olive oil is; however, they both have their own purposes. Coconut oil makes a better substitute for lard, shortening or butter in baking than olive oil does, and can be used topically as a skin cream. Olive oil is better for making salad dressing and other similar things.
Coconut Oil Vs. Palm Oil
Both coconut oil and palm oil come from palm trees; however, palm oil comes from the palm tree and coconut oil comes from the coconuts that grow on the coconut palm trees. Coconut oil is a far better environmental choice than palm oil is as to grow enough oil palm trees, virgin forests are being cut down to make room for them. Coconut oil is made from the coconuts that grow on coconut palm trees, while palm oil is made from the oil palm tree itself. Palm oil contains the same healthy medium chain fatty acids that coconut oil does, but in far less quantities. Palm oil contains high quantities of carotenoids, which are an excellent antioxidant; coconut oil also contains antioxidants. Coconut oil also contains antibacterial, antifungal and antimicrobial properties that palm oil does not contain. Palm oil is less expensive in price than coconut oil is, and is more readily available. However, palm oil is not as versatile as coconut oil is; palm oil is basically just a cooking oil, while coconut oil is a cooking oil, can be used in baking, is an excellent hair and skin care product, and can be taken for a daily health supplement. Between the two, palm oil is the least expensive choice, but coconut oil is the healthier choice.
Coconut Oil Vs. Flaxseed Oil
Flaxseed oil is made from flax seeds and much like coconut oil is a very healthy cooking oil. Flaxseed oil contains healthy omega-3 that coconut oil does not contain; it also contains thiamin, manganese, magnesium, fiber, copper, zinc, iron and calcium. Flaxseed oil also contains vitamin B6, niacin and vitamin K, plus trace amounts of vitamin E and C. Coconut oil only contains a small amount of vitamin K and E, and iron. Coconut oil contains healthy medium chain fatty acids like Lauric acid, Capric acid and Caprylic acid that flaxseed oil does not contain. Both flaxseed oil and coconut oil help to fight disease and help to maintain overall good health. Both are good cooking oils; however, coconut oil is more versatile than flaxseed oil is. Overall, coconut oil, is the healthier choice of the two.
Coconut Oil Vs. Sunflower Oil
Sunflower oil is made from sunflower seeds, while coconut oil is made from coconuts. Sunflower oil contains zinc, manganese, copper, magnesium, phosphorous, folate, calcium, potassium and iron. It also contains vitamins B1, B6 and B5, thiamine and vitamin E. In addition, it also contains trace amounts of vitamin C and A. Coconut oil does not contain a lot of vitamins and minerals; it only contains small amounts of vitamin K and E, and iron. Coconut oil contains healthy medium chain fatty acids like Lauric acid, Capric acid and Caprylic acid that sunflower oil does not contain. Sunflower oil helps to prevent a few health conditions like headaches, high blood pressure and indigestion; coconut oil helps to prevent disease like diabetes, heart disease, cancer, HIV and Alzheimer’s disease. Coconut oil also helps to boost the body’s immune system, increases the body’s metabolism and energy levels, and supports a healthy heart and thyroid. When compared on a health benefits level, coconut oil is the sure winner. Coconut oil is also more versatile than sunflower oil is; sunflower oil is basically only used as a cooking oil, while coconut oil is used for cooking and baking, as a daily health supplement and as a skin and hair care product. Sunflower oil is considerably less expensive than coconut oil is.
Coconut Oil Vs. Vegetable Oil
Vegetable oil is a variety of different oils combined together; it may contain corn oil, olive oil, peanut oil, safflower oil, sunflower oil, soybean oil and other edible oils. Vegetable oil is the most commonly used cooking oil in North America, as it is the least expensive and has the highest smoke point. However, vegetable oil is also one of the unhealthiest of all the cooking oils. Unlike most coconut oil, vegetable oil is extremely refined and contains a large amount of chemicals, additives and preservatives. While being refined, vegetable oil is heated to extremely high temperatures, which removes any nutritional properties it once had. Vegetable oil is high in omega-6, and has been proven to make the thyroid function improperly and causes a decrease in energy levels. Unlike coconut oil that is very versatile in its uses, vegetable oil really only has one use, a cooking oil. Vegetable oil is much less expensive than coconut oil is, but coconut oil is far better for a person’s health.
Coconut Oil Vs. Grapeseed Oil
Grapeseed oil is extracted from the seeds of grapes, while coconut oil is extracted from the meat of coconuts. Unlike coconut oil, which is thick and rich, grapeseed oil is light and thin. Grapeseed oil contains linoleic and oleic essential oils, and vitamin E. Grapeseed oil has a moderate amount of antioxidant properties. Both grapeseed oil and coconut oil are very stable oils and do not go bad quickly. Both grapeseed oil and coconut oil make good cooking oils, and are excellent for both the skin and hair. As grapeseed oil is thinner, it is easier to apply to skin than coconut oil is. Grapeseed oil is also preferred for cooking by some people, as it does not have a strong flavor like coconut oil has. However, when compared on a nutritional level, coconut oil is a healthier oil than grapeseed oil is.
Coconut Oil Vs. Fish Oil
Both coconut oil and fish oil are used to help with weight loss and to help maintain a healthy weight. Both fish oil and coconut oil are also commonly used to help promote overall good health. Both contain healthy fatty acids that help to promote a healthy heart and cholesterol levels. They also both help to promote healthy brain function. To get the benefits of fish oil, people can buy fish oil health supplements or can simply add fish to their diet at least twice a week. The best fish to eat to get fish oil from is tuna, herrings, sardines, salmon and whitefish. To get the health benefits of coconut oil, people can take it straight or it can be used as a cooking oil or in baking. Coconut oil is also commonly used topically, while fish oil is not.
MCT Oil Vs. Coconut Oil
MCT oil is also known as Caprylic and/or Capric triglyceride oil, medium-chain triglyceride oil or fractionated coconut oil. MCT oil is coconut oil that is processed in a way that removes all the long chain fatty acids in it, leaving only medium chain fatty acids. MCT oil contains very high levels of Caprylic and Capric acids, but does not contain any Lauric acid. MCT oil contains very high antioxidant and disinfecting properties. Generally, MCT oil is used to make medicine, soaps, hair care products, massage oils and other similar things. It can be used as a cooking oil like coconut oil, but due to its high price it is not an extremely popular cooking oil. Both MCT oil and coconut oil are very healthy oils and can be used topically as skin and hair care products, be used in cooking and baking, and make excellent daily health supplements.
Ghee Vs. Coconut Oil
Ghee is also known as clarified butter. Both ghee and coconut oil contain healthy fats and are safe for low-carbohydrate or ketogenic diets. Coconut oil is cholesterol free, while ghee contains 38 milligrams per tablespoon, so coconut oil is better for cholesterol levels. Coconut oil has more calories than ghee does so on the surface ghee is better for weight loss, but as coconut oil helps to promote healthy thyroid function and increases metabolism and energy levels, it also helps to promote weight loss. Overall, both ghee and coconut oil are healthy choices, but coconut oil offers more health benefits than ghee does. Coconut oil is also more versatile than ghee is; coconut oil is commonly used topically, while ghee is not.
Source: by Coconut Oil Facts
Full story: http://www.coconutoilfacts.org/coconut-oil-vs.php#
Disclaimer
The information contained on Coconutbenefits.com is intended for informational and educational purposes only. Any statements made on this website have not been evaluated by the Food and Drug Administration (FDA). Any information or products discussed on the website are not intended to diagnose, cure, treat or prevent any disease or illness. Please consult with your own health care professional before making changes to your diet. The website contains “affiliate links where appropriate.”
